 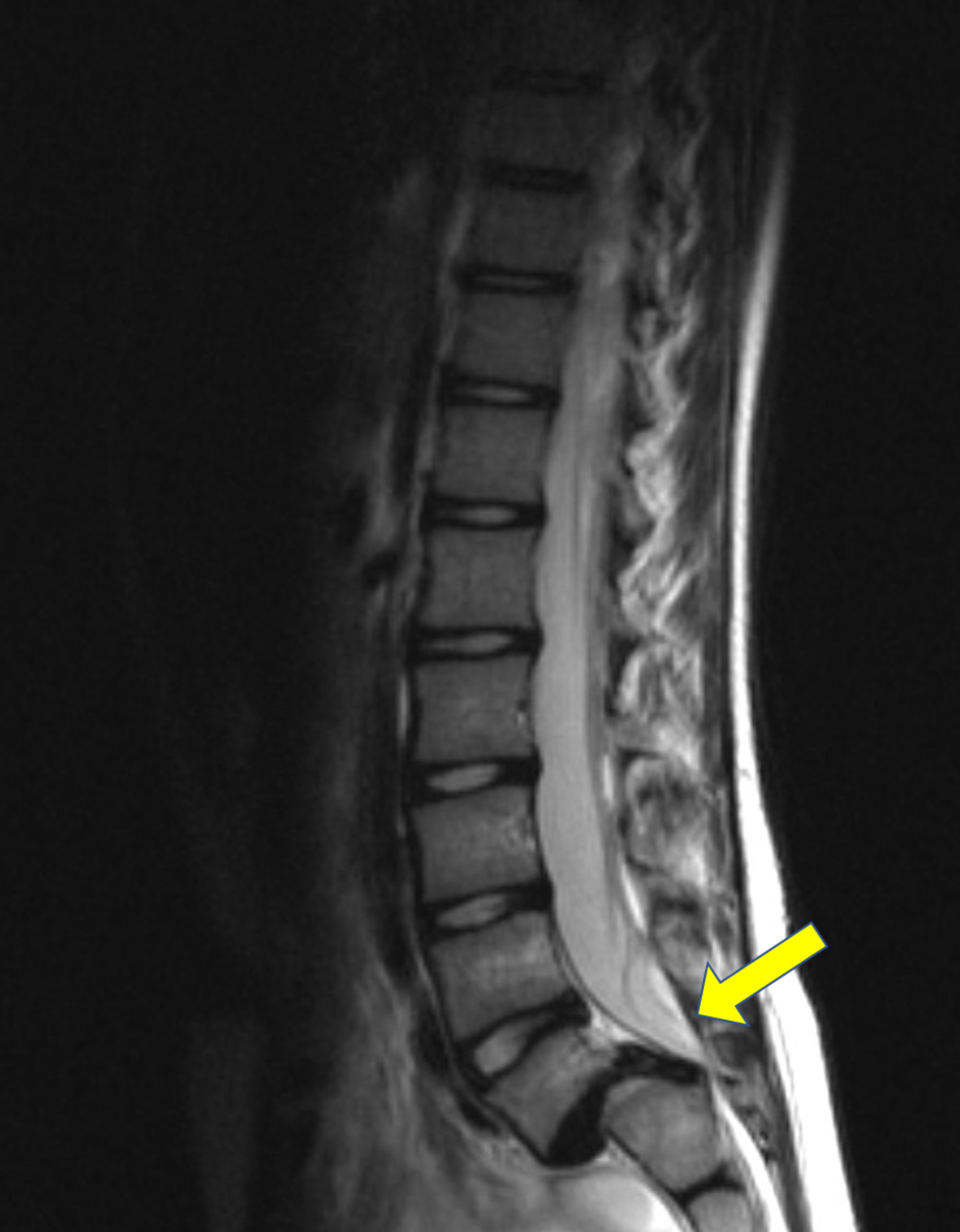
To determine if spondylolysis is the cause of your symptoms, your doctor may, in addition performing a physical exam, recommend a diagnostic test such as an x-ray, computed tomography (CT) scan or magnetic resonance imaging (MRI). Laboratory test results are normal in patients with one or both disorders. Range of motion is often not affected, but some pain can be expected on hyperextension. Sometimes there are mild muscle spasms and usually some local tenderness can be felt in the area. There may be a dimple at the site of the abnormality. Only when the slip reaches more than 50 percent of the width of the vertebral body will there begin to be a visible deformity of the spine. Often, the first physical sign of spondylolisthesis is tightness of the hamstring muscles in the legs. Many patients with spondylolisthesis will have vague symptoms and very little visible deformity. In this instance, there can be associated narrowing of the area where the nerves leave the spinal canal that produces irritation of a nerve root. In addition to back pain, patients may complain of leg pain. 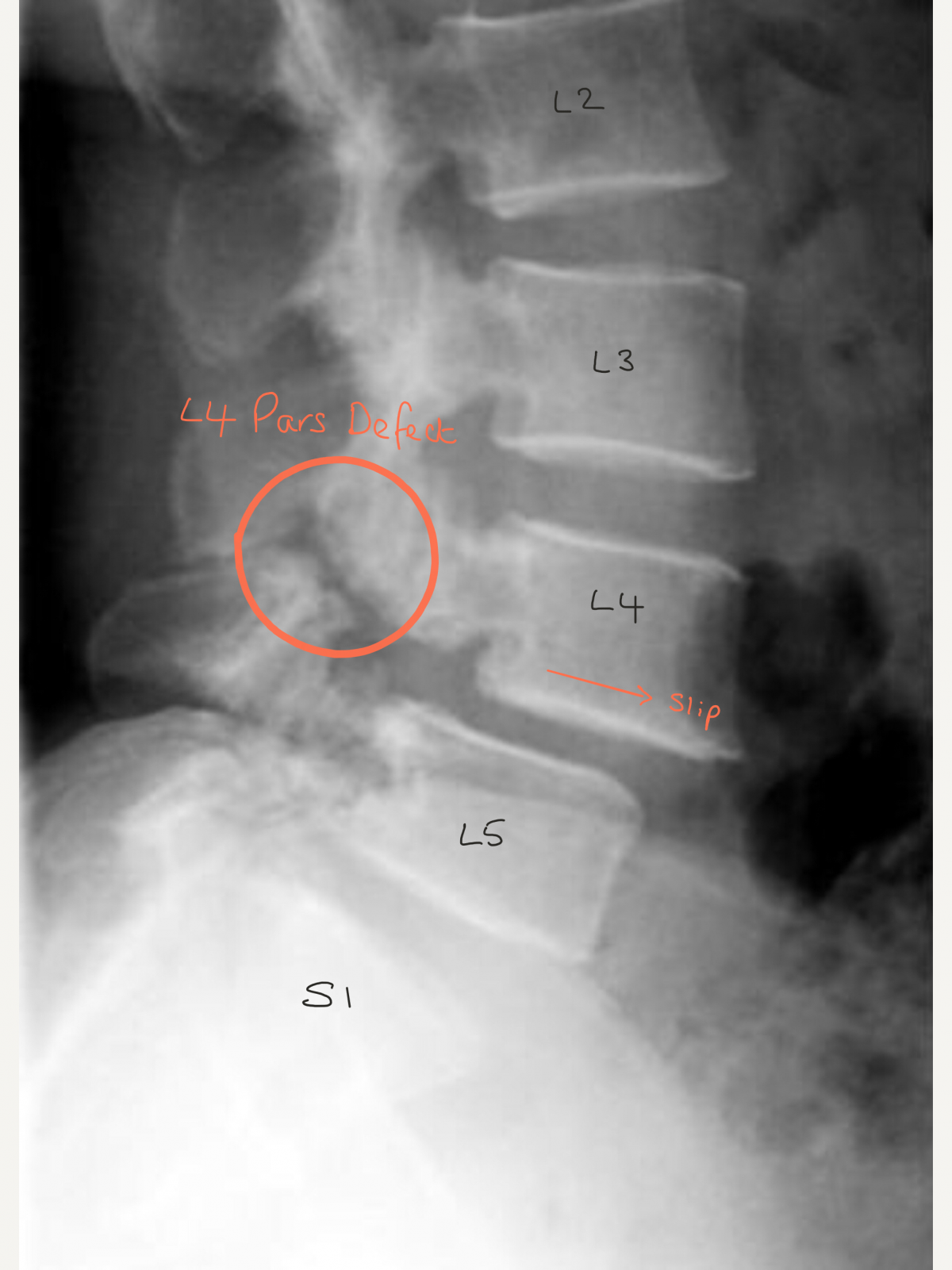
Fifty percent of patients with spondylolisthesis associate an injury with the onset of their symptoms. The degree of vertebral slippage does not directly correlate with the amount of pain a patient will experience. Usually the pain is relieved by extension of the spine and made worse when flexed. Many times a patient can develop the lesion (spondylolysis) between the ages of five and seven and not present symptoms until they are 35-years-old, when a sudden twisting or lifting motion will cause an acute episode of back and leg pain. The most common symptom of spondylolisthesis is low back pain. What Are The Symptoms Of Spondylolysthesis? Type V, pathologic spondylolisthesis, occurs because of a structural weakness of the bone secondary to a disease process such as a tumor or other bone disorder. Type IV, traumatic spondylolisthesis, is associated with acute fracture of a posterior element (pedicle, lamina or facets) other than the pars interarticularis. In Type III, degenerative spondylolisthesis there is no pars defect and the vertebral slippage is never greater than 30%. This type of spondylolisthesis is most often seen in older patients. The alteration in these joints can allow forward or backward vertebral displacement. Type III is a degenerative spondylolisthesis, and occurs as a result of the degeneration of the lumbar facet joints. Nuclear imaging may be needed to establish a diagnosis Type II C is very rare and is caused by an acute fracture of the pars.However, in contrast to Type II A, the pars interarticularii remain intact but stretched out as the fractures fill in with new bone Type II B probably also occurs from microfractures in the pars.It is also called a “stress fracture” of the pars interarticularis and is much more common in males Type II A is sometimes called Lytic or stress spondylolisthesis and is most likely caused by recurrent microfractures caused by hyperextension.Type II can be divided into three subcategories If one vertebra has slipped forward on the other (horizontal translation), it is considered spondylolisthesis. If a defect in the pars interarticularis can be identified but no slipping has occurred, the condition is termed spondylolysis. 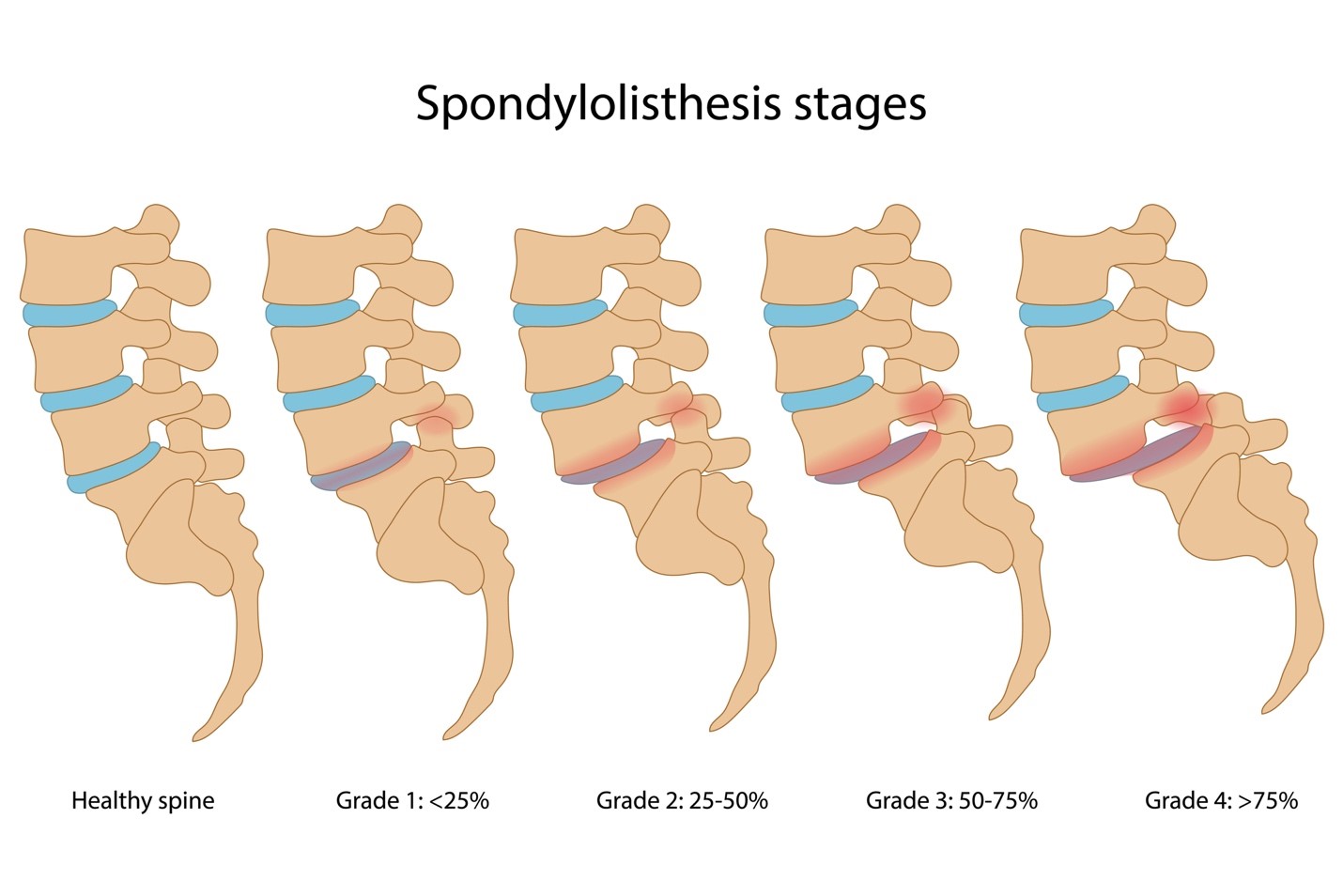
Type II, isthmic or spondylolytic, in which the lesion is in the isthmus or pars interarticularis, has the greatest clinical importance in persons under the age of 50. Type I is called dysplastic spondylolisthesis and is secondary to a congenital defect of either the superior sacral or inferior L5 facets or both with gradual slipping of the L5 vertebra. There are five types of spondylolisthesis 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
